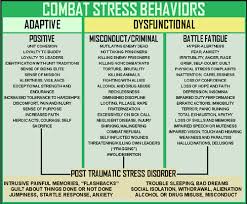
It is very natural and normal to have stress reactions after a traumatic or very upsetting event. Your behavior and emotions will change immediately afterwards and most people get better or find a ‘new normal’ after a few weeks. This is called acute PTSD. However, not everyone ‘gets over it’. As I discussed in the previous article PTSD, What is It? some people will have prolonged stress reactions to events and circumstances, most especially those that are more indicative of producing chronic PTSD. It is a real identifiable brain disorder (see picture).
Trauma causes REAL changes in the brain which can produce profound behavioral, emotional and physical symptoms. Please keep in mind as you read, the key to recognizing symptoms of PTSD is this: if it wasn’t there before a traumatic event happened and then appears, then there is a problem. If it was there before the traumatic event, then it most likely is not related to PTSD.
PTSD is generally diagnosed through presentation of 4 major types of symptoms that last longer than 3 months, cause you significant distress and disrupt your life and/or work.
Intrusion of the event into your life afterwards.
Recurrent recollections of the event. Memories coming back without warning with or without a ‘trigger’ (which I will discuss later)
Nightmares
Flashbacks/Reliving
These can make someone feel as though they are reliving the event in that MOMENT and can cause mental, emotional and physical symptoms. Some individuals with PTSD may experience and feel the same fears and horror as when the event took place.
Hyper Arousal/Feeling Keyed Up
Constantly on guard
Jittery/Jumpy
On Alert
Can’t relax
Can’t sleep
Numbing or Negative Changes in Beliefs and Feelings
Distancing self from people/Can’t trust other people
Unable to feel emotions
Forgetting about parts (suppression) or all of the traumatic experience
Not able to talk about the event
World becomes extremely dangerous
Depression/Anger/Irritability/Impending sense of doom
Avoidance:
Fear based and avoidance behavior typically involve all three of the above symptoms in order to avoid having to deal with the original trauma or prevent the above symptoms from occurring. Avoidance behavior is also another way of dealing with ‘triggers’. Often, people with PTSD will avoid people, places and things that remind them of the original trauma. Some people will get ‘super busy’ as way to avoid dealing with trauma.
Avoiding crowds
Avoiding driving
Avoiding all sorts of media (movie, news, video games)
Avoiding activities that are or could be associated with the trauma (ie an avid hunter may stop hunting to avoid particular triggers).
So this is the clinical take on what constitutes PTSD. But what can it really look like in someone’s life? It will vary from person to person obviously as everyone has different backgrounds, religious beliefs, personalities and different experiences in life. So lets look, in layman’s terms, what someone with PTSD may experience.
Panic Attacks or other anxiety problems including hypersensitivity to his/her surroundings….this is experience of INTENSE fear which most often is accompanied by shortness of breath, sweating, nausea, dizziness and racing heart. At the very least, discomfort may occur. This is almost directly related to hyper vigilance and may be ‘triggered’ by something totally unrelated to what is happening in that very moment.
Feelings of mistrust (could be specific or not)
Problems in daily living: not being able to function ‘normally’ at work, home and within relationships. This can include a decline in personal hygiene (or obsessiveness with it). Stopping doing daily household chores, organizational problems, etc. Emotional distancing of themselves towards other people, places and things in order to cope with feeling ‘unsafe’. This can come across as being cold, aloof, uncaring, demanding or otherwise socially unacceptable behaviors.
Substance Abuse: using drugs or alcohol to cope with emotional pain
Depression/Mood Swings: persistent sadness, anxiety, emptiness, loss of interest, guilt, shame, hopelessness about the future. Going from being happy to angry and back again for no real apparent reason. Isolating themselves. May become aggressive and angry for ‘no good reason’.
Memory problems are almost always present. Usually this shows up at first as ‘absent mindedness’ such as constantly misplacing things or loosing things. It can progress into forgetting names, appointments and other day to day things. Later on, someone with PTSD may even begin to forget past events that were important to them, or forget what they were saying in the middle of a sentence and may even say something and then repeat themselves a few minutes later.
Risk Taking Behavior such as driving too fast, multiple sex partners, starting fights and other behaviors that typically would be considered ‘risky’ with the potential to do harm to themselves or others.
Isolating from the world…many people with PTSD will in an effort to keep themselves safe begin to withdraw from people to the point that they may turn into ‘recluses’ who only go out when food or medicine is needed.
Obsessive/Compulsive Behaviors: check and rechecking that a door is locked, driving around and around in a parking lot, running to the doctor every time they sneeze. The point in obsessive/compulsive behavior to keep themselves ‘safe’ to prevent further trauma.
Super sensitivity to outside stimulation: this is directly related ‘triggers’. When the original traumatic event occurs, the brain basically ‘burns’ into the deepest part of the memories and cortex exactly what happened, how it happened and circumstances in which it occurred.
Checklist of PTSD symptoms:
Physical Symptoms:
Headaches
Stomach problems
Changes in breathing patterns (shortness of breath/not breathing normally)
Lack of energy OR Hyper Activity
Sleep problems
Emotional pain never felt before
Anxiety problems
Hypersensitivity
Hyper vigilance
Psychological Problems:
Mood swings
Memory problems
Addiction/Self Medication
Loss of personal hygiene/housekeeping
Risk taking behavior
Isolation
Depression (“what’s the point?”)
Paranoid thoughts
Reliving the event(s) with accompanying emotions
Sleep Problems:
Insomnia (not being able to fall asleep or stay asleep)
Having nightmares
Waking up covered in sweat
Kicking during sleep
Constantly waking up and falling back asleep
Waking up and being easily startled and/or being confused about where you are
Irregular sleep cycles
It is my hope that you have found this information helpful in describing what PTSD ‘looks’ like symptomatically. Too often many seek help and a diagnosis of PTSD is not given because the full spectrum of what PTSD looks like isn’t known by many doctors and mental health professionals. Do not be afraid to print this off and take it with you if you choose to seek help (which I hope you will) so that you maybe appropriately helped and treated. PTSD is multi-faceted and can be difficult to diagnosis unless you and those around you know the facts about what it is and what it looks like. But it is treatable and can be overcome. There is hope.
In part 3 of this series on PTSD I will discuss ‘triggers’ which plays an important role in PTSD.
Survivingshtfmom